Back to All Clinical Evidence
![]()
![]()
![]()
![]()
![]()
![]()
 PUBLICATION_
PUBLICATION_  PUBLICATION_
PUBLICATION_ 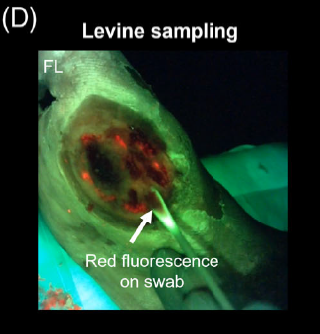 PUBLICATION_
PUBLICATION_
Accelerated Wound Healing, Accelerated Wound Healing
Routine fluorescence imaging to detect wound bacteria reduces antibiotic use and antimicrobial dressing expenditure while improving healing rates: Retrospective analysis of 229 foot ulcers
Related Publications
Accelerated Wound Healing
Accelerated Wound Healing
Related Material
 PUBLICATION_
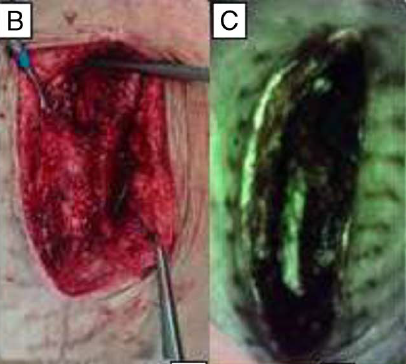
PUBLICATION_ Multidisciplinary Strategies With Real-Time Fluorescence Images and Negative Pressure Wound Therapy to Manage Organ/Space Surgical Site Infection in Transplanted Kidneys
 PUBLICATION_
PUBLICATION_ Assessing Pediatric Burn Wound Infection Using a Point-of-Care Fluorescence Imaging Device
 PUBLICATION_
PUBLICATION_ Lights, fluorescence, action—Influencing wound treatment plans including debridement of bacteria and biofilms
MolecuLight Headquarters
425 University Avenue
Suite 700
Toronto, ON M5G 1T6
Canada
US Address
MolecuLight Corp.
2403 Sidney Street,
Suite 286
Pittsburgh, PA 15203
T.
+1 647-362-4684
North American Toll Free:
1-877-818-4360
F.+1 647-362-4730
E:
info@moleculight.com
Sitemap
©2026
The MolecuLight® i:X and MolecuLightDX™ Imaging Devices are approved by Health Canada for sale in Canada and has CE marking for sale in the European Union.
The MolecuLight™ i:X and DX Imaging Devices have received FDA clearance.










