Abstract
Early diagnosis of wound-related cellulitis is challenging as many classical signs and symptoms of infection (erythema, pain, tenderness, or fever) may be absent. In addition, other conditions (ie, chronic stasis dermatitis) may present with similar clinical findings. Point-of-care fluorescence imaging (MolecuLight i:X) detects
elevated bacterial burden in and around wounds with high sensitivity. This prospective observational study examined the impact of incorporating fluorescence imaging into standard care for diagnosis and management of wound-related cellulitis. Two hundred thirty-six patients visiting an outpatient wound care centre between January 2020 and April 2021 were included in this study. Patients underwent routine fluorescence scans for bacteria (range: 1-48 scans/patient). Wound-related cellulitis was diagnosed in 6.4% (15/236) of patients. In these patients, fluorescence scans showed an irregular pattern of red (bacterial) fluorescence extending beyond the wound bed and periwound that could not be removed through cleansing or debridement, indicating the invasive extension of bacteria (wound-related cellulitis). Point-of-care identification facilitated rapid initiation of treatments (source control and antibiotics, when warranted) that resolved the fluorescence. No patients had worsening of cellulitis requiring intravenous antibiotics and/or hospitalisation. These findings demonstrate the utility of point-of-care fluorescence imaging for efficient detection and proactive, targeted management of wound-related cellulitis.
Back to All Clinical Evidence
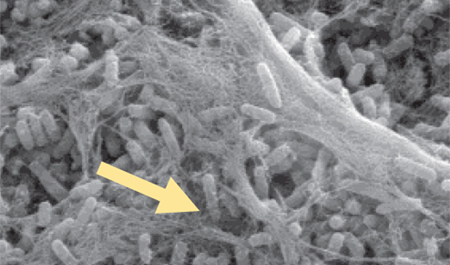
Species Detected/Biofilm, Acute Wounds
Diagnosis and treatment of the invasive extension of bacteria (cellulitis) from chronic wounds utilising point-of-care fluorescence imaging
Efficient, accurate diagnosis of cellulitis critical to avoid costly complications
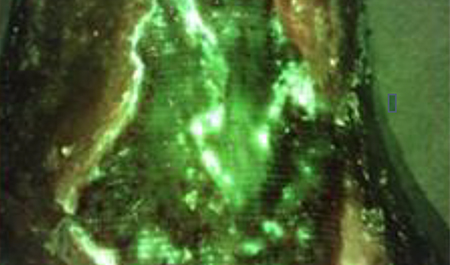
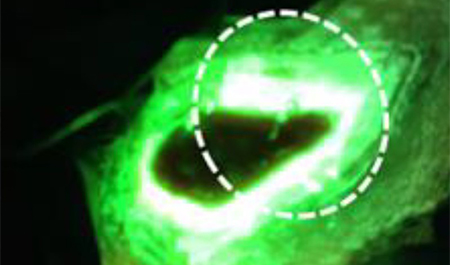
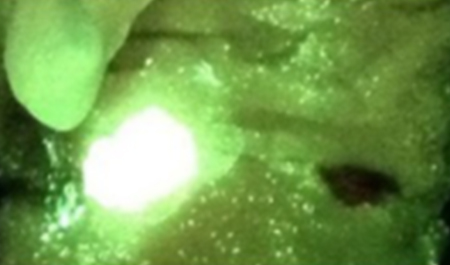
Unique pattern of red fluorescence extending beyond the wound was observed in all cases of wound-related cellulitis
Fluorescence imaging aided in the early diagnosis of wound-related cellulitis, resulting in the initiation of oral antibiotics without delay, avoiding progressive cellulitis